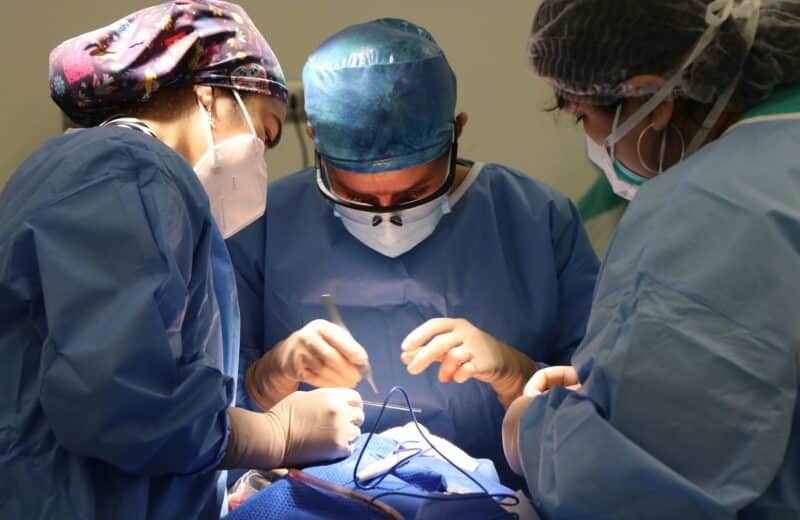
Source: Columbia University Mailman School of Public Health
Researchers at the Center for Infection and Immunity at Columbia University’s Mailman School of Public Health have identified distinct immune changes in patients diagnosed with chronic fatigue syndrome, known medically as myalgic encephalomyelitis (ME/CFS) or systemic exertion intolerance disease.
The findings could help improve diagnosis and identify treatment options for the disabling disorder, in which symptoms range from extreme fatigue and difficulty concentrating to headaches and muscle pain.
These immune signatures represent the first robust physical evidence that ME/CFS is a biological illness as opposed to a psychological disorder, as well as the first evidence that the disease has distinct stages. Results appear online in the new American Association for the Advancement of Science journal, Science Advances.
With funding to support studies of immune and infectious mechanisms of disease from the Chronic Fatigue Initiative of the Hutchins Family Foundation, the researchers used immunoassay testing methods to determine the levels of 51 immune biomarkers in blood plasma samples collected through two multicenter studies that represented a total of 298 ME/CFS patients and 348 healthy controls.
They found specific patterns in patients who’d had the disease for three years or less that were not present in controls or in patients who’d had CFS for more than three years. Short-duration patients had increased amounts of many different types of immune molecules called cytokines.
The association was unusually strong with a cytokine called interferon gamma that’s been linked to the fatigue that follows infection with many viruses, including the Epstein-Barr virus (the cause of infectious mononucleosis). Cytokine levels were not explained by symptom severity.
“We now have evidence confirming what millions of people with this disease already know — that ME/CFS isn’t psychological,” says lead author Mady Hornig, M.D., director of translational research at the Center for Infection and Immunity and associate professor of epidemiology at Columbia’s Mailman School. “Our results should accelerate the process of establishing the diagnosis after individuals first fall ill, as well as discovery of new treatment strategies focusing on these early blood markers.”
There are already human monoclonal antibodies on the market that can dampen levels of a cytokine called interleukin-17A, which is among those the study shows were elevated in early-stage patients.
Before any drugs can be tested in a clinical trial, Dr. Hornig and colleagues hope to replicate the current, cross-sectional results in a longitudinal study that follows patients for a year to see how cytokine levels, including interleukin-17A, differ within individual patients over time, depending on how long they have had the disease.
Stuck in high gear
The study supports the idea that ME/CFS may reflect an infectious “hit-and-run” event.
Patients often report getting sick, sometimes from something as common as infectious mononucleosis (Epstein-Barr virus), and never fully recovering. The current research suggests that these infections throw a wrench in the immune system’s ability to quiet itself after the acute infection, to return to a homeostatic balance; the immune response becomes like a car stuck in high gear.
“It appears that ME/CFS patients are flush with cytokines until around the three-year mark, at which point the immune system shows evidence of exhaustion and cytokine levels drop,” says Dr. Hornig. “Early diagnosis may provide unique opportunities for treatment that likely differ from those that would be appropriate in later phases of the illness.”
The investigators went to great lengths to carefully screen participants to make sure they had the disease. The researchers also recruited greater numbers of patients whose diagnosis was of relatively recent onset. Patients’ stress levels were standardized; before each blood draw, patients were asked to complete standardized paperwork, in part to engender fatigue.
The scientists also controlled for factors known to affect the immune system, including the time of day, season, and geographic location where the samples were taken, as well as age, sex, and ethnicity/race.
In 2012, W. Ian Lipkin, M.D., director of the Center for Infection and Immunity, and colleagues reported the results of a multicenter study that definitively ruled out two viruses thought to be implicated in ME/CFS: XMRV (xenotropic murine leukemia virus) and murine retrovirus-like sequences (designated pMLV: polytropic MLV). Drs. Hornig and Lipkin expect to report the results soon for a second study of cerebrospinal fluid from ME/CFS patients.
In separate ongoing studies, they’re looking for “molecular footprints” of the specific agents behind the disease–be they viral, bacterial, or fungal–as well as the longitudinal look at how plasma cytokine patterns change within ME/CFS patients and controls across a one-year period, as noted above.
“This study delivers what has eluded us for so long: unequivocal evidence of immunological dysfunction in ME/CFS and diagnostic biomarkers for disease,” says Dr. Lipkin, senior author of the current study and the John Snow Professor of Epidemiology at Columbia’s Mailman School. “The question we are trying to address in a parallel microbiome project is what triggers this dysfunction.”
(This information provided courtesy of Columbia University Mailman School of Public Health. Co-authors are Andrew F. Schultz, Xiaoyu Che, and Meredith L. Eddy at the Center for Infection and Immunity; Jose G. Montoya at Stanford University; Anthony L. Komaroff at Harvard Medical School; Nancy G. Klimas at Nova Southeastern University; Susan Levine at Levine Clinic; Donna Felsenstein at Massachusetts General Hospital; Lucinda Bateman at Fatigue Consultation Clinic; and Daniel L. Peterson and Gunnar Gottschalk at Sierra Internal Medicine.)
(WhatDoctorsKnow is a magazine devoted to up-to-the minute information on health issues from physicians, major hospitals and clinics, universities and health care agencies across the U.S. Online at www.whatdoctorsknow.com.)