By Tom Mullaney
We live in a time of technology disruption. Airbnb has revolutionized the rental markets model. Uber and Lyft have impacted the taxi industry, which, depending upon how you look at it, is either a good or a bad thing. Technology is similarly poised to disrupt healthcare.
Healthcare has been slower than other industries, such as retail and banking, to adopt digital technology. While there are a few options available today, such as Fitbit and Jawbone, they are geared toward tracking fitness and activity levels. When it comes to more complicated physiology, patients remain the passive recipients of medical treatments and advice from doctors in medical settings.
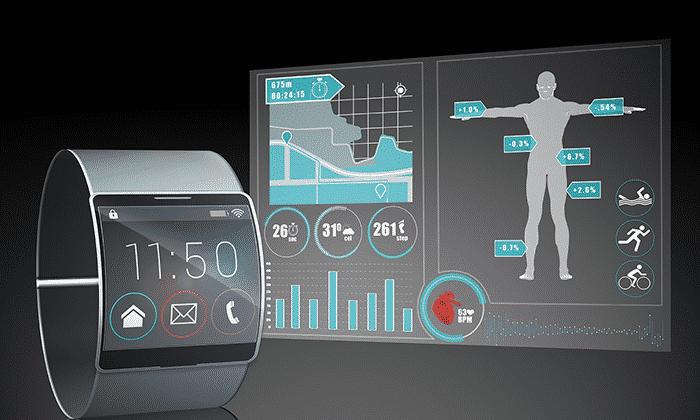
But the industry is on the verge of a brave new world that will turn tales out of science fiction into science fact. The proliferation of medically useful apps and wearables—smart watches and clothing equipped with microsensors—will soon give patients much greater power over their health decisions.
Fitbit, Jawbone and similar monitors are apps’ first-generation stage. Under development are apps and wearable sensors that will be able to track a wearer’s physiology and mood in real time, manage chronic diseases and intervene to keep a patient from backsliding behavior or prevent an emergency.
ABI Research has projected that, by 2016, wearable wireless medical device usage will exceed 100 million devices. Last July, Google struck a partnership deal with Swiss drugmaker, Novartis, to commercialize a prototype contact lens by 2020 that will monitor glucose levels in one’s tears. In England, Parkinson’s UK is funding trials of up to 3,000 patients testing a smartphone app’s ability to detect persons with Parkinson’s based on signals in their voice, gait, posture and reaction time to commands. It has registered a 99 percent accuracy rate.
Locally, Chicago has been behind the curve in healthcare innovation, but things are changing. MATTER, an entrepreneurship and innovation hub, has raised more than $4 million from private investors and named an initial group of 20 health tech start-ups that will share space at MATTER’s offices in the Merchandise Mart.
“Chicago has a dynamic start-up community, world-leading healthcare companies, research institutions and medical associations,” says Steven Collens, MATTER CEO. “By bringing the entire community together to fuel greater collaboration and innovation, MATTER hopes to accelerate the development of next-generation healthcare technologies.”
The hot spot for such innovation is now in predictive analytics. Physicians and hospital health systems are currently unable to meaningfully interpret the reams of data generated by medical devices. A fertile field thus exists for start-ups to enter the analytics arena.
Companies and medical researchers are developing killer apps, which, combined with a software technology platform, can take big data and break it into actionable diagnostic and therapeutic patterns. The three disease populations attracting the most research are heart failure, COPD (chronic obstructive pulmonary disease) and diabetes.
Gary Conkright, CEO of PhysIQ, a predictive analytics company in Naperville, has launched a technology platform designed to detect subtle changes in vital signs and physiologic indicators. It can construct a personalized health baseline for any patient, therefore, offering greater sensitivity and quicker physician intervention than general population baselines.
Conkright calls the coming transformation of healthcare “Quantified Medicine 2.0,” the ability to detect subtle but significant changes in patient health before the first symptoms appear or up to a week prior to a medical event such as a stroke or heart attack.
PhysIQ currently is monitoring 50 congestive heart failure patients in a study at four veterans affairs hospitals and, this month, started a study of 25 COPD sufferers in a private physician practice.
“There is increasing clinical evidence of the value of continuous physiological data in managing chronic diseases and monitoring patients posthospitalization,” says Theo Ahadome, senior analyst at IMS Research.
Another analytics start-up is Qualia Health Inc., founded by David Bieser, MD, an assistant professor of medicine at the University of Chicago Medicine and Kevin O’Leary, a graduate student at the University of Chicago Booth School of Business. Qualia provides at-home monitoring of heart failure patients in-between physician visits.
Qualia has had success in the past year engaging major health providers for its evidence-based app. It will soon complete a 90-day pilot study tracking the at-home physical and emotional health of 25 L-VAD (left ventricular assist device) patients, some awaiting a heart transplant, at Northwestern Memorial Hospital (NMH). Qualia will also soon begin supporting studies at additional hospitals, including Stanford University Hospital.
Last October, Qualia announced a collaboration with the American Heart Association. They are building software to help cardiovascular disease patients better manage their health between doctor visits. The software tracks 12 physical, mental and social domains of heart health—anxiety, depression, blood pressure and social isolation—over a 90-day period and provides patients with personalized feedback. Pilot studies are set to begin early in 2015 at a handful of hospitals.
Patient intervention by a device that communicates with both patient and physician is another frontier for innovation. Bonnie Spring, a professor of preventive medicine and director of the Center for Behavior and Health at Northwestern’s Feinberg School of Medicine, is part of a team working on integrated technologies (sensor to app to electronic health record) to promote better health behavior.
Doctors know that changing of ingrained behavior patterns is hard. A high percentage of patients remove their wristbands and stop exercising or taking their medications at some point after they return home from the hospital.
Spring was recently awarded a $10.8 million grant from the National Institutes of Health to develop wearables that will keep patients from relapsing into unhealthy behavior related to smoking and obesity.
“Our approach differs from existing apps in that we don’t believe people are necessarily aware of the times when they’re most at risk of lighting up or overeating,” Spring says. “We’re developing just-in-time interventions that learn about a patient’s daily routines and habits to know when they’re at risk even before they know it themselves.”
Sensors, still in development, would identify signals, like respiration, heart rate, sweat gland activity, wrist movements and change of location. Wrist movements and change of location might signal reaching for a cigarette or going outside to smoke. Patients could then receive a signal or email suggesting a healthier alternative to lighting up or eating that donut.
Qualia’s O’Leary tells how its intervention helped a heart patient. His sensor captured his level of well-being falling from 80 percent to 10 percent over a three-day period. The latter data indicated a state of clinical depression. Qualia immediately notified the patient’s doctor. After the doctor called and spoke with the patient, his well-being level returned to 80 percent.
Asked where health technology might be in five years time, O’Leary says, “Where I hope it will be is that you will be able to access your medical data just like your doctor [can]. You will be on an equal footing and more involved in your own treatment. Medical data will be personalized and in patients’ hands so that you and your doctor will have a more collaborative relationship than the one that exists now.”
Lyle Berkowitz, MD, is the associate chief medical officer of innovation for NMH and director of the Szollosi Healthcare Innovation Program. He says, “Technology can help in early detection, tracking and education of patients, but it’s important to remember this should be in supporting the doctor-patient relationship, not replacing it.”
So, when your doctor tells you to “wear your medicine,” he or she isn’t joking. +
Originally published in the Winter/Spring 2015 print edition