By Paul Huddleston, M.D., Tribune Content Agency
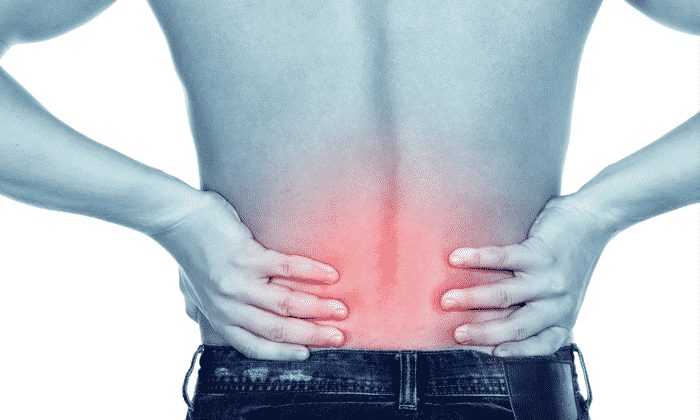
DEAR MAYO CLINIC: I have osteoarthritis in my spine. About a month ago, I got a steroid shot in my lower back because my doctor said it might help with stiffness and pain in my back and legs. It worked wonderfully, and my symptoms are gone now. How does this medicine work? If the pain comes back, could another one of these shots take care of it again? Or is my arthritis gone?
ANSWER: The injection you received likely contained a corticosteroid medication. These powerful drugs can be very useful in treating many conditions that cause joint pain, including osteoarthritis.
How long the effects of a corticosteroid injection last can vary quite a bit, depending on your health and the severity of your symptoms. If your pain returns, you may be able to get another injection. Because of the possibility of serious side effects, though, the number of injections and how often you can receive them is limited. Unfortunately your arthritis is not gone, even if you’re not currently having any symptoms.
A corticosteroid shot helps relieve joint pain by decreasing inflammation in and around a joint. They’re used in people who have osteoarthritis because the disease frequently leads to joint pain, tenderness and swelling, especially in the hands, knees, hips and spine. The injections also are commonly prescribed for people who have pain due to other disorders, such as tendinitis, carpal tunnel syndrome, gout, bursitis and rheumatoid arthritis, to name just a few.
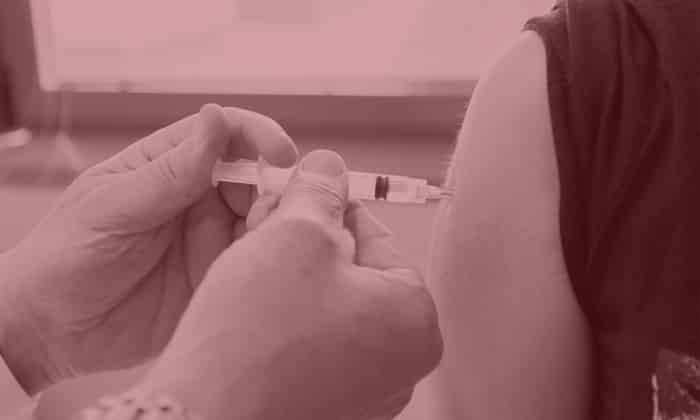
Getting a corticosteroid shot usually involves only an office visit to your doctor. Before the injection, the area around the injection site is cleaned. Your doctor may apply an anesthetic spray to numb the area where the needle is inserted. To make sure the needle is placed correctly, your doctor may use ultrasound or a type of x-ray called fluoroscopy to watch where the needle goes inside your body.
After the needle is inserted, the medication is released into the injection site. Typically, these shots include the corticosteroid medication to relieve pain and inflammation over time, as well as an anesthetic to provide immediate pain relief.
How long the pain relief from a corticosteroid injection lasts depends a great deal on your individual health situation. For some people, the effects may last only a week or two, while others may be symptom-free for several months or more.
Corticosteroids can be very effective in relieving symptoms such as joint pain, tenderness and stiffness, but they’re not without risks. For some people, the shot may cause a flare of pain and inflammation in the joint just after it’s given. In most cases, these symptoms fade within 48 hours of receiving the injection.
Although uncommon, longer-lasting complications can include nerve damage, joint infection, damage to nearby tendons, and thinning of the bones near the injection site. There are some individuals who have temporary pain relief due to the numbing medicine commonly used with these shots, but they don’t obtain long-term pain relief. Additionally, people who take blood thinners for the treatment of stroke, heart or clotting disorders may not be able to have the injections safely while on those medications.
There is some evidence that repeated corticosteroid shots do not change the way arthritis in the spine progresses over time. Chronic use of the shots eventually can cause cartilage within a joint to deteriorate, resulting in permanent joint damage. Because of that, these injections are usually not given more often than once every six weeks. It’s also typically recommended that people receive corticosteroid injections no more than three or four times a year.
If you notice your symptoms of osteoarthritis returning, review the benefits and risks of a second corticosteroid injection with your doctor to help decide if another shot may be the right choice for you. — Paul Huddleston, M.D., Orthopedic Surgery, Mayo Clinic, Rochester, Minn.
(Mayo Clinic Q & A is an educational resource and doesn’t replace regular medical care. E-mail a question to MayoClinicQ&A@mayo.edu. For more information, visit www.mayoclinic.org.)