3D printing could be the answer to better replacements
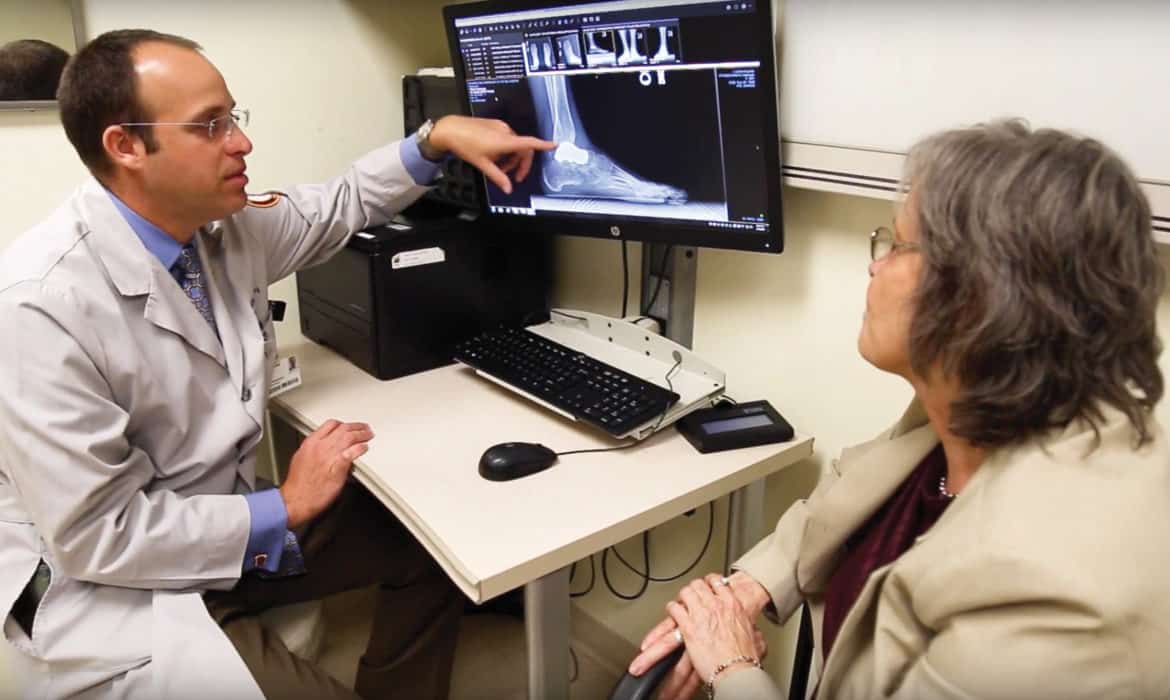
In 2017, Deborah Stoneburner was driving back from the Illinois State Fair in Springfield when a horrific accident occurred. She and her boyfriend struck a tree near their home, and Stoneburner suffered numerous injuries, including a crushed talus.
The talus is the primary link between the lower leg and the foot, and it’s crucial for mobility. The injury left Stoneburner unable to walk and on the hunt for treatments.
Several options were presented to Stoneburner to get her walking again, including fusion, replacement with a cadaver bone and even amputation. However, none were ideal — fusion would have caused her to lose an inch or two of height on one side, a cadaver bone could be rejected by her body and amputation meant losing one of her feet.
Then Stoneburner learned about 3D-printed bone replacements at Loyola University Medical Center. And in January 2018, she became the first Loyola patient to receive a 3D-printed talus.
Printing new bone
Stoneburner’s surgery was done by Loyola orthopedic surgeon Adam Schiff, MD, who says 3D printing is revolutionizing the field.
“3D printing opens a real world of possibilities that have never been there before — especially with the talus,” Schiff says. “I think we’re just scratching the surface of what we can do.”
Schiff modeled Stoneburner’s replacement talus after the intact bone in her other ankle. By customizing the replacement to Stoneburner’s existing bone structure, he was able to have greater confidence that the replacement would be a perfect fit.
Stoneburner’s cobalt chromium talus wasn’t covered by insurance, and it cost her about $13,000. But it’s a price that was worth it, she says. The replacement has allowed her to walk again and to return to the active hobbies she enjoyed before her accident.
Orthopedic advancements
“From a biomaterial standpoint this is a golden age for orthopedics,” says Wellington K. Hsu, MD, a professor of orthopedic surgery at the Northwestern University Feinberg School of Medicine. Hsu, who is studying regenerative therapies for bone healing, is also looking at the early stages of 3D printing for spine implants.
“We 3D print scaffolds that can regenerate bone [provided they have] the right amount of human material,” Hsu says. The scaffold acts as a base that living cells can attach to as they evolve into tissue.
For patients who suffer from degenerative disk disease, fractured vertebrae or herniated disks, these 3D-printed scaffolds would be implanted into the spine to heal and strengthen existing bone material. Currently, such patients must undergo invasive spinal fusions, which involve fusing two bones together to heal into a single, solid bone. Using Hsu’s technology, which is undergoing animal testing, new bone would grow in the space without the need to fuse bones together.
Hsu says a reliable technology for regenerating bone could be extremely beneficial for patients, especially since spinal fusions can fail.
“It could decrease reoperation rates,” Hsu says. “Hopefully these technologies will be better than what we already have, because, for many patients, their bone is of insufficient quality” to support a fusion.
Optimizing replacements
At DuPage Medical Group, Aakash Chauhan, MD, is using 3D templating software for shoulder replacements. The software creates a digital model of a patient’s shoulder that can then be used to improve the accuracy of implant positioning during surgery.
“It helps me improve my accuracy on the glenoid, or ‘socket,’ of the shoulder,” Chauhan says. “Accurate placement of instrumentation in the glenoid can be one of the most important and challenging parts of shoulder replacement surgery. If the glenoid implants are not placed correctly, then the replacement can have a high chance of failure.”
3D printing opens a real world of possibilities that have never been there before.”
The template starts with a CT scan, the results of which are uploaded onto a computer. From there, the surgeon can optimize the replacement based on the size and position it needs to fit into, as well as a patient’s individual anatomy and arthritic condition. Custom, patient-specific instrumentation and intraoperative guides are additional tools that can help improve the accuracy of implant positioning.
The 3D printing process allows for much better accuracy for shoulder replacement surgeries, which is good news, as Chauhan anticipates that more people will need shoulder replacements in the future as our society ages.
Overall, physicians anticipate that 3D printing and bone regeneration technologies will continue to alleviate many of the challenges patients face today. Those improvements include better positioning of replacement parts, extending the longevity of the replacement bone, limiting reoperations and regenerating bone that will allow for better healing.
The search is ongoing for beneficial materials for replacement parts. Hsu says he anticipates a day when replacement parts will have the capability to aid a patient in other potentially life-saving ways, including delivering antibiotics to eradicate infections and preventing bacteria from attaching to the part.
“There’s a huge interest and need to find materials that are compatible with the human body,” Hsu says. And, with so much promise, 3D printing might be a bone-shaking development.