Having reproductive choices doesn’t always mean having control over your body
Last fall, I asked my healthcare provider to switch my generic birth control prescription from a Target to a Walgreens that was more convenient. I went to pick up the medication, only to find that with the pharmacy change also came a change in generic pill. I didn’t give it too much thought. At age 37, I’d been taking the pill off and on for a couple of decades, and never had any noticeable side effects. So I popped the blister pack and made my way around the circle of pills.
The changes started slowly. There were some tears here and there—uncharacteristic, but not unheard of. Then came the out-of-the-blue tension with my boyfriend. On top of it all, I felt overwhelmed by work. By January, 120 days in, all of the above had escalated, and I could actually taste my anxiety, it was so high. On a Friday, I stopped taking the pill.
By Sunday I could feel the difference. My hot blood cooled to a mellow mountain stream. As time passed, the calmness continued. Today marks more than four months without tears, arguments or that taste of anxiety. As someone who’s always felt—illusion or otherwise—in control of my body, it’s been a wake-up call to the power of hormones.
Sabrina Holmquist, MD, says that every woman responds differently to different birth control methods, and what works for me might not work for my sister or my best friend. As an associate professor of obstetrics and gynecology at University of Chicago Medicine who specializes in contraceptive care for medically complicated patients, she emphasizes to her patients that there are myriad options out there, and sometimes it takes trying more than one to find the right fit. While a certain pill may negatively impact my mood, it might mean less moodiness and less bloating for someone else.
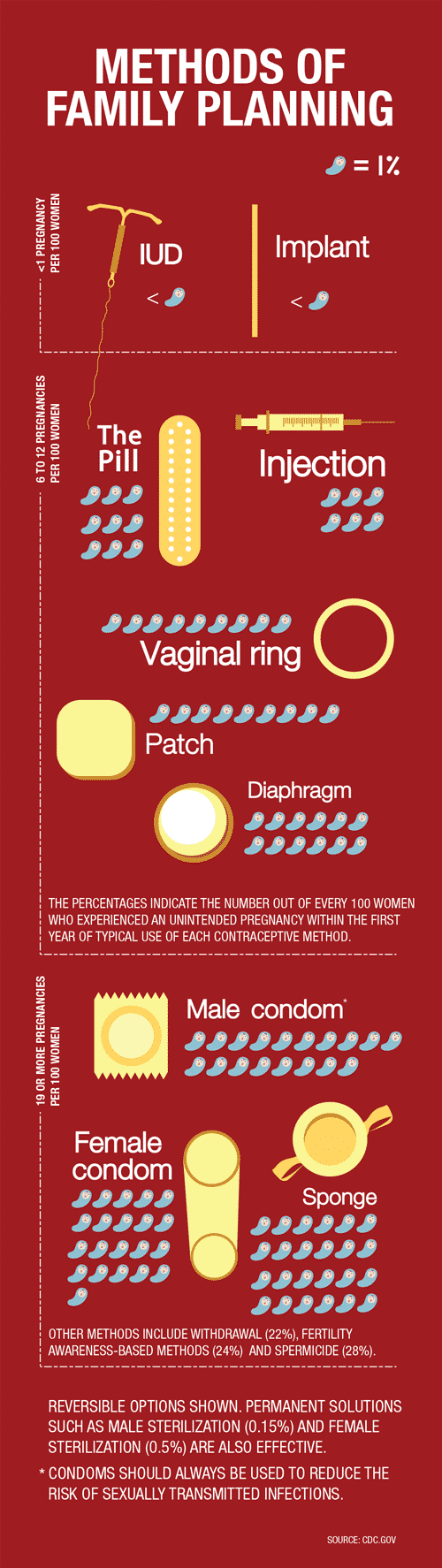
“The good news is, we have so many different methods, you can almost always find something that is going to really jibe with an individual’s contraceptive needs and how she experiences contraception in her life. There’s lots more birth control than just pills,” Holmquist says. “At the end of the day, the most important thing is that you don’t wind up with a pregnancy that you weren’t intending.”
There are two hormones frequently seen in birth control: estrogen and progesterone. Both are made in the ovaries and are associated with ovulation and menstruation, and both carry their own possible side effects.
Teresa Tam, MD, an OB/GYN with All for Women Healthcare, says that most birth control pills and the vaginal ring (which a woman inserts once a month) are a combination of estrogen and progestin—a synthetic version of progesterone—while a number of other methods are progestin only. Those include the Mirena IUD (which is inserted in the uterus and is effective for up to five years), Nexplanon contraceptive implant (which is inserted in the arm and is effective for up to three years), Depo Provera (an injection that prevents pregnancy for three months) and so-called “mini pills,” which are birth control pills without estrogen.
Tam says that some people who opt for progestin-only methods can’t tolerate estrogen, while others are postpartum moms who are breastfeeding, and estrogen will decrease breast milk production. There are also nonhormonal options, such as ParaGard, the hormone-free copper IUD (a T-shaped device that sits in the uterus, releasing copper, which prevents sperm from reaching a woman’s eggs), male and female condoms, the sponge, diaphragms and spermicides—all barrier methods. And then there are permanent solutions: for men—vasectomy (cutting or blocking the vas deferens, which carry sperm); and for women—tubal ligation (closing or blocking the fallopian tubes).
Both Tam and Holmquist say they’ve been seeing a dramatic increase in what’s referred to as “long-acting reversible contraception” in recent years, particularly the IUD. Women who choose that method tend to appreciate its low-maintenance nature and the convenience factor: It takes just one medical visit for insertion, which then lasts three to 10 years. There are two types of IUD to choose from: nonhormonal (ParaGard, the copper IUD) and hormonal (Mirena and Skyla, which both release a small amount of progestin).
Whatever method you choose, Tam says she advises patients to be, well, patient. “Give it a three- or four-month trial,” she says. “Your body has to get accustomed to it.”
Holmquist adds that it’s important to be open with your doctor—and yourself—about what method makes the most sense. If you have trouble remembering to take a daily pill, for example, try another method. “I think the most important thing to remember is that the best contraceptive for any individual is the one that she’s going to use,” she says.
For me, personally, the hormone experience was a wake-up call. I have the utmost respect for the pill and what it’s done for women, but my next birth control method, whatever it may be, will be hormone-free.