With federal Medicaid and SNAP cuts looming, safety-net hospitals brace for an uncertain future
Fact checked by Jim Lacy
Mount Sinai Hospital on Chicago’s West Side is bright and busy early on a Thursday morning. People stream through the entrance. Security guards greet regulars and hand out badges to visitors.
This is not the Sinai that leads the 10 p.m. news.
“One of the things that people don’t get about safety-nets like Sinai: They hear about us on the news, when gunshot victims come into our Level-1 trauma center,” says Dan Regan, vice president of communications and marketing at Sinai Chicago. “They think: Mount Sinai and trauma, gun violence.”
Inside, the building feels like home.
Nelly Garcia, one of the city’s few licensed clinical social workers dedicated to the emergency room, has worked here for nearly a decade. Each morning, she stops in the lobby first, scanning for anyone who might be looking for her — someone who needs shelter, food, or protection.
The work, she says, is a calling.
“I am who I take care of. I am Little Village. I am Lawndale. I am Roseland and Humboldt Park,” Garcia says. “There is no better type of social work than to be with my people on the frontline when they’re most vulnerable.”
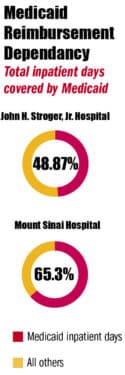
That’s who safety-net hospitals serve — in Chicago neighborhoods and across rural Illinois. Sinai, the state’s largest private safety-net hospital, treats 150,000 patients a year. Roughly 70% rely on Medicaid, and 9% are uninsured.
Cook County Health, the state’s largest public safety-net system, served about 200,000 people in 2025 and delivered 40% of the county’s charity care. “That number was $280 million last year. We budgeted $380 million this year,” says Chief Executive Officer Erik Mikaitis, MD.
Illinois counted 34 safety-net hospitals in 2025, according to the state Department of Health and Family Services. That number fell to 33 after Weiss Memorial Hospital closed this past August.
“Safety-net hospitals are critical anchors to the entire healthcare ecosystem,” says Sinai Chicago CEO Ngozi Ezike, MD.
Yet, no single definition governs safety-net status. The label typically reflects ownership, Medicaid volume, and uncompensated care.
They also employ thousands. Sinai Chicago has roughly 3,500 workers. Cook County Health has about 7,000.
Both systems now are facing federal policy shifts that threaten their financial footing.
Three looming losses
The One Big Beautiful Bill Act, known as HR1, includes sweeping Medicaid cuts and changes to the Affordable Care Act.
One immediate impact: federal tax credits that helped subsidize marketplace plans expired at the start of 2026. Mikaitis says out-of-pocket costs rose by an average 95% for those affected.
Next year, a second challenge will take shape as Medicaid work requirements begin. Enrollees must document at least 80 hours of work or volunteer activity per month. How states will implement or monitor those requirements remains unclear at the federal level.
Evidence from states that have already implemented work requirements raises concerns.
When Arkansas launched its Medicaid work requirements in 2018, the state spent about $26 million in the first year to run the program. Within seven months, roughly 18,000 people lost coverage. Research found that 97% of the targeted population already met the requirements — mostly because they were working or had a disability — so the policy did not significantly change employment. Many people lost coverage because of reporting and paperwork barriers, not because they were ineligible.
“It has shown itself to be more of an exercise in creating paperwork barriers [than in] maintaining coverage,” Mikaitis says.
Georgia spent $54 million to administer a program delivering $26 million in health coverage. “Imagine if you could just spend that money on actually providing healthcare,” he says.
A third challenge is more frequent redetermination. Instead of verifying eligibility annually, Medicaid beneficiaries must do so every six months.
“It’s again — much like work requirements — increasing paperwork burden,” Mikaitis says.
The timing is precarious. Federally qualified health centers (FQHCs) have announced layoffs. Some hospitals have closed; others are in trouble.
“Barring some intervention, we’re going to see additional hospitals closing, and that’s going to create a cascade,” Mikaitis says.
During the next eight years, an estimated half a million Illinois residents could lose coverage. The Congressional Budget Office projects that 11.8 million people nationwide will become uninsured as Medicaid spending drops by $911 billion.

Ezike sees two likely outcomes. Some people will continue seeking care but pay out of pocket. Others will delay treatment.
“For our self-pay patients, we don’t even collect 2 cents on the dollar,” she says. Those who delay care “will be in the ER in a much sicker state with a more expensive stay. However you slice it, it makes for a sicker community and further strains all hospital systems.”
Many people have been ignoring the warnings. They have private insurance. They rarely visit safety-net hospitals. They assume the changes won’t affect them.
Ezike disagrees.
“If you’re driven not by the fact that healthcare is something everybody should have and everyone is healthy as a result, fine. Then let’s think of it in a self-interested sort of way,” she says. “Your hospital will have longer wait times. Those people that you are not concerned about [right now], they will have to access your hospital if theirs is shut down.”
And in emergencies, every second counts — whether it’s your health crisis or someone else’s.
When minutes matter
In Sinai’s neonatal intensive care unit, nurses move quietly among 21 bassinets. The Level III NICU, licensed for 32 beds, cares for the area’s sickest newborns. Many stay for months.
“When we speak to the need within the community, there is no doubt there is a need,” says Laura Griffith Gilbert, director of women’s and children’s services.

Hari Srinivasan, MD, an attending neonatologist, recalls a recent winter night when temperatures plunged to minus-20 degrees. Four miles north, a woman delivered her baby in a gas station bathroom.
The full-term infant quickly developed hypothermia.
Emergency medical services transported the baby to Sinai. By arrival, the infant’s core temperature had fallen to 33.5 degrees.
“We were able to warm up the baby,” Srinivasan says. The child developed pulmonary and cardiac complications, all successfully treated. “But if we didn’t have this ICU in this area — if you’re going to spend another five, 10, 15 minutes in an ambulance — that’s crucial time.”
Chicago has an oversupply of beds, he says, but not in the right places.
Births in Illinois have declined sharply — from 180,000 in 2000 to 125,000 in 2025. That drop prompted closures of labor and delivery units, especially on the South and West sides.
In rural Illinois, closures will likely have a bigger impact. The shuttering of any single hospital means people will have to drive significantly farther for medical care.
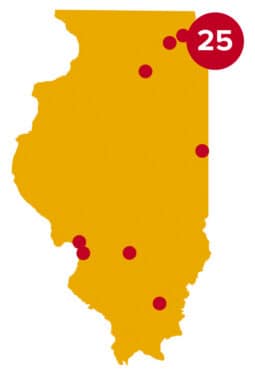
Researchers at the University of North Carolina who study rural health services say nine Illinois rural hospitals risk closure under the new Medicaid and ACA changes:
• OSF Sacred Heart Medical Center in Danville
• Hoopeston Community Memorial Hospital in Robinson
• Crawford Memorial Hospital in Robinson
• Richland Memorial Hospital in Olney
• Harrisburg Medical Center in Benton
• Franklin Hospital in Benton
• Massac Memorial Hospital in Metropolis
• Hardin County General Hospital in Rosiclare
• Katherine Shaw Bethea Hospital in Dixon
“What’s coming is deeply concerning,” Miklaitis says.
At Sinai, staff focus on what they can control. Srinivasan and Gilbert know the cost of each NICU bed (about $50,000) and each ventilator (roughly $20,000). Renovating a labor and delivery room can cost up to $150,000.
So they take care of what they have and encourage others to do the same.
They also focus on dignity. “We work really hard to make moms feel veryspecial,” Gilbert says. When a baby leaves the NICU, the staff hold a graduation ceremony so families can celebrate milestones often overshadowed by fear.
A legacy of access
Ten minutes Northeast of Sinai sits John H. Stroger, Jr. Hospital, part of Cook County Health and the nation’s oldest and largest public hospital.
“Anyone who comes to us, if you need help, we’re here for you, regardless of immigration status, regardless of insurance,” Mikaitis says.
Cook County Hospital opened in 1857 to serve the Irish, German, and Italian immigrants who built Chicago’s sewers, railroads, and skyscrapers. Crowded tenements fueled outbreaks of cholera, smallpox, scarlet fever, typhoid, and tuberculosis. The hospital responded to all of them, as well as the 1918 influenza, polio, and HIV/AIDS.
On the first floor of the original hospital building, now largely repurposed as a hotel, a small museum traces that history. A quote from Louis Pasteur, the 19th-century chemist who transformed modern understanding of infectious disease, stretches across one wall: “One does not ask of one who suffers: What is your country, and what is your religion?” The words distill the hospital’s founding ethos.
Yet, today’s immigrants, who still power the city’s economy, increasingly fear seeking care. They see videos on social media of federal agents detaining people, and they worry that they could be next — even if they’re citizens, even if they’re seeking medical care.
Fear at the front door
Mount Sinai’s emergency department on any given afternoon is an orchestra of machines beeping. One afternoon, Michael Casner, MD, assistant medical director of Mount Sinai Hospital’s emergency department, and Jhoanna Gulmatico, system director of emergency departments, describe the palpable shift.
“Patients are sheltering. They’re afraid to come to the ED unless they’re really sick,” Gulmatico says. “They’re not coming in for [asthma] treatments. They’re coming in later when they now need advanced airway support.”

Middle photo: Neonatologist Hari Srinivasan, MD, and Laura Griffith Gilbert, director of women’s and children’s services, stand among babies in Sinai’s neonatal ICU.
Bottom photo: Michael Casner, MD, assistant medical director of Sinai’s ER at the department’s main desk.
Photos by Katie Scarlett Brandt
Even before immigration enforcement intensified, many people used emergency departments as their primary care providers because they had no other options.
“Patients come to us because [primary care] is not available to them, unfortunately,” Gulmatico says. “They treat the ED as their primary care clinic, which then leads to an inefficient way of caring.”
Casner sees more than 15 patients in a typical eight-hour shift; on busy days, up to 20. Chest pain, abdominal pain, hypertension, and diabetes dominate.
“For our patient population, they’re sometimes deciding between: Can I afford my medication vs. my electricity vs. food for my family?” he says. “Choices that a lot of other people don’t even have to think about, things that would be world-shattering for other people.”
Sinai also serves neighborhoods with some of the city’s highest rates of violence. Staff call summer “trauma season.” Yet most patient visits involve medical, not traumatic, conditions. This year, Sinai’s trauma cases are down 15%, which aligns with a 17% drop in gun violence citywide.
“It shows that violence prevention programs and getting the community involved help,” Casner says.
Even with a positive trend, uncertainty looms. “Are hospitals like us going to be able to stay open?” he wonders. “Where are our patients going to go?”
Gulmatico feels responsible for protecting workers and patients. “It’s my day-to-day reality,” she says. “How do I carry the team? How do I plan ahead?”
Aging buildings, deferred dreams
In Sinai’s basement, Brian Piejko, system vice president of facilities operations, design and construction, and real estate, manages a different vulnerability: infrastructure. The hospital’s first building opened in 1919; the newest wing dates to the 1980s. Temperature swings strain aging systems.
“Two weeks ago, we were fighting frozen pipes. This week, we’re fighting people feeling hot,” Piejko says. “We don’t have modern infrastructure that can shift heating to cooling right away.”
Boilers, electrical systems, and climate controls compete with CT and MRI scanners. “If we can’t supply good electricity, what’s the point of getting a good CT scanner?” Piejko asks.
Well-resourced hospitals replace systems on schedule. Safety-nets often defer upgrades.
“You’re forced to budget and plan based on have-to as opposed to want-to,” Regan says.
Every five years, Sinai conducts a facilities assessment across its 1.5 million square feet. Piejko and his 27-person team project needs for one, three, five, and 10 years out.
“When you don’t have that consistent money, things get deferred,” he says.
“A lot of times we’re doing fire drills.”
In that way, Sinai’s brick and mortar reflect the state in which its patients often arrive at the hospital: worse off than they might be if they could keep up basic maintenance.
That’s part of what drew Piejko to Sinai two years ago. “I just felt like the place needed my help,” he says. “Every patient deserves a good place to heal, regardless of where they live.”
Searching for solutions
Thirty minutes west in Oak Park, West Suburban Medical Center, also a safety-net hospital, has been fighting its own battle after the closure of its sister hospital, Weiss Memorial Hospital in Chicago, which closed its doors in 2025. This past March, the hospitals’ CEO, Manoj Prasad, announced that West Suburban would halt its patient operations due to a financial crisis and subsequently suspended services indefinitely, effectively closing the facility.
“People think of safety-nets as a catchall for the poor,” says Terry Tuohy, who oversaw medical education at both Weiss and West Suburban.
Solutions, she argues, must be multifaceted. “Big institutions could come together with the safety-net hospitals. There needs to be collaboration. The state needs to be at the table.”

She envisions structured collaborations in which well-resourced hospital systems near a safety-net facility provide financial support, staffing, or best practices. Rural hospitals need similar state-backed arrangements.
Mount Sinai President Sameer Shah, PharmD, calls safety-net work both a privilege and a burden. “It takes a lot more resources to care for people who are underserved,” he says.
A person in an affluent area may have family members who can provide transportation to appointments and to the pharmacy. A patient at Sinai or other safety-nets may face housing insecurity, unreliable transportation, and no insurance.
“You can’t just discharge a patient with nowhere to go,” Shah says.
Meanwhile, reimbursement often runs at a fraction of commercial rates. “We’re getting reimbursed at significantly lower rates compared to other organizations, but we still provide the same standard and level of care,” Shah says. “That’s the beauty of Sinai — people doing 10 times the amount of work to take care of these patients with a fraction of the resources.”
The question now is sustainability. “How can we do this for two years, five years, 10 years more?” he asks.
At Cook County Health, leaders have launched a Medicaid work group that includes academic medical centers, business leaders, philanthropists, and government agencies. The Greater Chicago Food Depository has joined discussions about pairing food distribution with medical visits.
“Can we give people an option to see their doctor when they’re picking up food?” Mikaitis asks.
Internally, Cook County Health has tightened budgets, adjusted schedules, and explored partnerships to avoid job losses while bracing for increased charity care.
Ezike, who previously led the Illinois Department of Public Health during the Covid-19 pandemic, continues to reach out to better-resourced institutions. “Our health is all interconnected,” she says. “If you don’t have healthy individuals, you can’t have a healthy workforce. If you’re not healthy, you can’t have a productive school environment. We’re the building blocks.”
She says she tries to stay hopeful, but, “Unfortunately, I’ve seen this movie; I’ve read this book,” she says, referring to the pandemic. “I was in the movie — where you see the people not caring as much as you’d want them to for other people.”
Mikaitis echoes the concern. When rural or safety-net hospitals close, those patients “start going out to other places,” he says. “People who aren’t close to it may think it’s a problem down the street or across town. That’s in fact not the case. It is going to affect all of us. Costs will go up, wait times will increase, and we’ll have a sicker population that won’t be able to work.”
If they show up at Sinai’s ER, social worker Nelly Garcia will be waiting for them. She’ll log into the system and scan every patient — why they came, what risks they face, who might need protection.
“This tells me from my own lens who I need to prioritize,” she says. “If there are concerns on my end that they’re getting trafficked [or being abused], how do I keep them safe?”
Garcia has spent a decade in this department and a lifetime in the neighborhoods it serves. She worries about what deep funding cuts could mean.
“I don’t know that our hospitals can take such a massive hit,” she says. “We’re there for the community. If we can’t do that, then where else are people going to get their care?”
For now, she continues her rounds — offering comfort after hard diagnoses, arranging shelter, holding hands through dialysis. As long as her community needs her, she plans to be there.
Originally published in the Spring/Summer 2026 print issue.

An award-winning journalist, Katie has written for Chicago Health since 2016 and currently serves as Editor-in-Chief.











