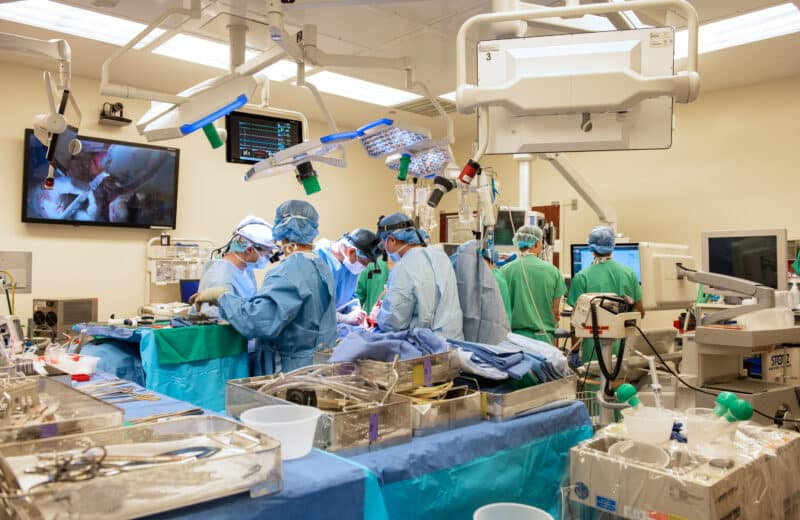
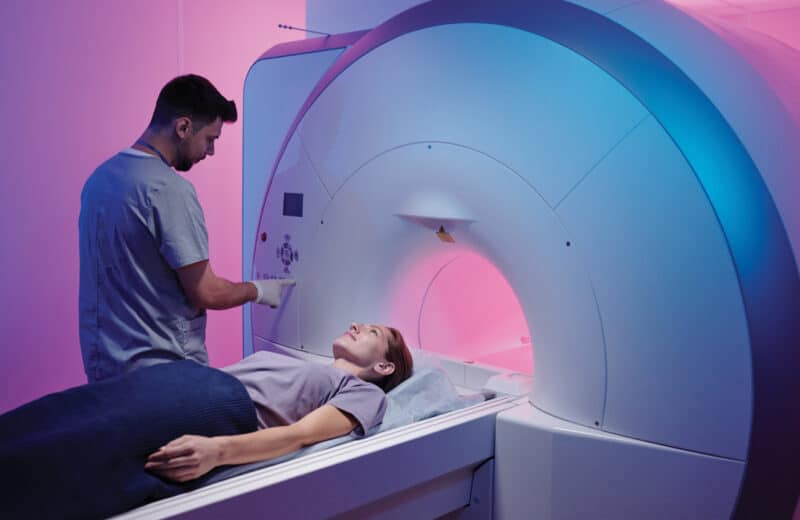
In a shifting healthcare landscape, where do you find the best and most practical care? And how in the world do you pay for it?
Healthcare is a complicated business. And an expensive one. But never before has it been this complex. The intricacies of our healthcare ecology have extended into nearly every other aspect of our society.
It used to be simpler.
You had a family doctor, and you and your family went to see him or her whenever something wasn’t as it should be. The emergency room was for, well, emergencies. And the hospital was a place where babies were born and the most dire health problems were faced. A steady paycheck or employer-sponsored benefits afforded your insurance, and your insurance paid for your healthcare. The system worked. But that was then.
Today the cost of healthcare has skyrocketed, outpacing the ability of employers and individuals to keep up with it. In 2011, the rate of uninsured Americans rose to 17.1 percent according to Gallup. And even higher rates of minorities live without the protection of coverage. More than 40 percent of Hispanic Americans have no health insurance at all.
The country’s emergency rooms are full of nonemergencies; patients who have no insurance and no primary care doctor and don’t know where else to turn. In many cases, the patient has neglected an ailment for as long as possible until immediate care is the only option. This approach to one’s healthcare is the most expensive and damaging option, yet it is increasingly common. We need a smarter and more affordable approach. The well-being of our bodies and our economy demand it. And we may be getting closer to it.
Avoiding the Doctor
Ever experience the frustration of arriving at your doctor’s appointment the day after your symptoms subside? It’s kind of like trying to explain to the mechanic that the car’s been making noise for a week while it idles quietly in the background.
A case of, “well, it’s not doing it now.”
Most of us are healthy, most of the time. But everyone gets an unexpected visit by some hostile bacteria or virus on occasion. When these maladies don’t clear up on their own, and it’s time to call in the pros, a visit to the doctor’s office may not be the most affordable or practical option today.
Retail clinics are conveniently sprouting up throughout Chicagoland. You can swing into one during your weekly errand run. In models, like those employed by the Take Care Clinics in select Walgreens and Minute Clinics at certain CVSs, getting checked out is as simple as tossing a bar of soap into your shopping cart.
People are able to “just walk right in when they’re feeling ill and get seen [by an advanced nurse practioner],” says Audrey Collins, market manager at Take Care, who oversees clinic operations for the Chicago region.
At the back of the store next to the pharmacy you’ll find an electronic kiosk, where you can sign up to be seen and view a menu of services and treatments along with the correlating cost. “Transparency” is the word Collins uses repeatedly to describe the upfront pricing.
Traditionally, the emergency room was the only place people thought of when seeking immediate, walk-in healthcare services. But the last decade or so has seen an enormous rise in the number of walk-in options.
The RAND Corporation found that in two years, visits to retail health clinics rose tenfold (between 2007 and 2009). And multiple studies show cost savings of up to 80 percent when visiting a walk-in clinic over an emergency room.
One of the fastest growing healthcare models is actually one that’s been around for quite some time. Immediate-care hospitals like Concentra have long provided occupational medical services. In fact, workman’s compensation-related procedures remain the core of Concentra’s business. But a growing number of patients are going to Concentra instead of the ER. And occasionally, even instead of their primary care physician.
With locations in major cities throughout the country, Concentra provides access to hospital-level care in non-life-threatening situations. They have a team of permanent physicians, they don’t require an appointment and they’re far more affordable than the emergency room.
“Don’t forget, when you go to the emergency room you’re being billed for the room itself, in addition to the services,” says Dr. Kimberly Dettloff, regional medical director for Concentra in the Chicago area.
At Concentra, much like Walgreens, the cost of care is displayed up front. A menu in the lobby of the Franklin Park clinic breaks down pricing in blocks, by level of care. But unlike many walk-in clinics, Concentra is equipped with trauma rooms and X-ray equipment as well as the necessary qualified staff on hand.
Cherie Varzino, the center’s operations director at the clinic in Franklin Park, says the goal is to “get you what you need, so you can get on with your life,” describing the everything-under-one- roof approach at Concentra.
The three trauma rooms at the Franklin Park clinic serve as a “mini ER,” says Varzino. “Anything that’s not life or limb threatening, they can handle… lacerations, burns, foreign body removals—[some of] the gory stuff.
“There’s a lot of overhead when you have a staff of emergency room doctors, who are taking care of bronchitis and lacerations, Dettloff says. “Things we can [treat] at our level free up [ER docs] to do what they need to do.” And Detloff says reducing the cost of staffing will drive costs down for everybody.
Anything that requires significant follow-up should be taken to your primary care doctor, but Concentra is “a very nice option for young healthy people who don’t necessarily need to have a primary care doctor at their beck and call,” says Dettloff.
“All of our centers are staffed with docs who are there everyday,” she says. “We’re not taking care of long-term issues, but as things come up, we know your history, we know who you are as a person. It’s an extension of what we’ve been doing for a long time.”
Illinois Bone & Joint Institute (IBJI) has been doing what they do for a long time as well. But recently, they’ve recognized the growing demand for immediate care and launched their OrthoAccess program at the Glenview, Gurnee and Libertyville locations. Melody Winter-Jabeck, administrator of IBJI Glenview–Wilmette division, describes it as the orthopedic answer to urgent care. You don’t need an appointment, and they’re open until 8 p.m. Monday through Thursday, until 6 p.m. on Friday and from 8 a.m. to noon on Saturday. Two more of IBJI’s more than 20 locations are scheduled to bring OrthoAccess online this year. And they’re eyeing even greater expansion of the program.
“Because of what we do, we’ve always seen a fair amount of patients on a same-day basis,” explains Winter-Jabeck.
Dealing in fractures and sprains, IBJI is accustomed to the need for immediacy. But, in the past, traditional hours have left a lot of patients heading for the ER.
“It’s really ingrained,” says Winter-Jabeck, “this idea that if you have something that can’t wait until the doctor’s office opens, you go to the emergency room. For years we’ve been shaking our heads when people go to the emergency room for an ankle sprain.”
Now, it’s easier than ever to be seen at IBJI, and it’s clear it’s making a difference. Winter-Jabeck says about 60 percent of the patients who fill out a survey at the OrthoAccess clinics say that if they hadn’t come to IBJI, they would have gone to the ER.
Specialized Care
Long-term acute care (LTAC) is something most people don’t think about— and thankfully don’t need to. But catastrophic illness or injury can strike, and family members have to make the call as to where their loved ones will be cared for after they’ve been stabilized at the hospital.
Acute care hospitals, the kind most of us think about when we think of a hospital, find it more difficult and expensive to provide long-term treatment because of their multi-disciplinary nature and the necessity for a high patient-turnover rate.
“We’re the bridge between the very intense care that takes place in a hospital and the complete recovery stage,” says Dr. Maria Iliescu, medial director at Kindred Hospital Chicago North.
“Patients are here until they get better and are able to transition home, to a rehab center or to a nursing home.”
Jeanne Valencia was hospitalized after a cold turned into pneumonia and sent her into respiratory failure. Like almost all of Kindred’s patients, Valencia already had complex pre-existing conditions that made it much harder for her than a healthy personto recover from an illness. After Valencia was stabilized at the hospital, her son knew she would want the family to do everything they could to get her back home. He asked Kindred for help.
“We see our patients on a daily basis; we have a multidisciplinary team involved in every case,” says Iliescu. “We have consultants such as pulmonologists—like myself, and consultants in infectious disease, nephrology, hematology, cardiology…” In fact, Kindred has over 250 specialty doctors on its team available for consultations.
“They work so well together,” Valencia says to me on the phone from her home over the sound of the Cubs game on her TV. As I acknowledge the interdisciplinary team of physicians at Kindred, Valencia cuts me off, “I’m not even talking about the doctors.” The doctors receive high marks from
Valencia, but she says it’s “the regular everyday people who work there. They interact with the patients in a way you don’t see in a lot of hospitals.”
At an LTAC, like Kindred, the time needed for recovery is one of their specialties. The average stay at Kindred is 25 to 30 days. “The joy of practicing at Kindred is that you have the chance to see [patients] coming off the ventilator,” says Iliescu.
Due to the length of a patient’s stay in an LTAC, the relationship with the healthcare providers is all that much more important. Valencia describes the day her physical therapist took her outside of the hospital. “That was one of the turning points for me,” Valencia says. “Remembering the wind and the sun.”
Her family came to Kindred with the goal of sending Valencia home. Together, with the team at Kindred, they achieved that goal. Valencia tells me she can go on and on about how pleased she is, but at another time. The Cubs are on.
Reaching The Underserved
The University of Illinois Hospital and Health Sciences System is a leader in caring for Chicago’s underserved communities. And as an academic hospital, it is able to bring those patients up to the frontlines of medical advancement. Dr. Joe G.N. Garcia, vice president for health affairs, sees no better way to make healthcare more effective.
“Everyone’s talking about personalized medicine these days, but they’re not really talking about personalized medicine for Latinos or African Americans,” Garcia says. “This is something we’re specifically focused on. [Using] genomic and genetic strategies to understand individual risks and individual responses to therapies [among minority populations], we have a better shot of reducing healthcare costs down the road and delivering better care.”
The University of Illinois Hospital and Health Sciences System has long focused on caring for underserved communities. It recently rebranded itself with the longer moniker, carefully adding the word “system,” to let people know that its more than just a medical center.
“We’ve identified [locations] within our primary service area that are areas of need and have partnered with schools to provide care within and actually have built a neighborhood community clinic under the Mile Square umbrella,” says Garcia.
Mile Square Health Centers are federally qualified community health centers. In the South Shore neighborhood, a predominantly African American and historically blighted area of the city, a Mile Square clinic conveniently located in a strip mall off of 71st Street and Jeffrey Boulevard strives to connect with its community.
“The majority of our patients, maybe 75 to 80 percent, are Medicaid patients,” says Mallari Peace, a nurse practitioner at the Mile Square clinic.
“People who are privately insured are using many different strategies to obtain their healthcare,” says Garcia. “The patients we take care of, even having access to a primary care physician is sometimes problematic.”
At the South Shore Mile Square, “we do a really good job of [handling] child care visits; making sure kids are up-to-date on their immunizations,” says Peace, as well as providing guidance on nutrition; a growing importance in the face of rising rates of obesity and diabetes.
While obesity has become a national epidemic, and diabetes affects people across all socioeconomic borders, there are major disparities. According to the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) and the American Diabetes Association; 14.7 percent of all African Americans aged 20 and older suffer from diabetes, compared with 9.8 percent of all Caucasians in the same age range.
Peace says she asks patients about what they’re eating. And spends a lot of time talking to young parents about the food they buy, helping them to understand that they’re “setting the habit for what their kids will be [eating] as they grow older.
“I find that patients are very concerned about weight now and eating healthfully,” says Peace. But the problem is often a financial one. “The food that isn’t the healthiest is so inexpensive and the easiest to buy.”
However, there are economic reasons for both patient and hospital to focus on preventative care, particularly in the University of Illinois Hospital and Health Sciences System model, with a majority of patients on Medicaid. Reimbursements for providers are frankly not that good. And the state’s bureaucracy slows the flow of money.
“The incentives are not aligned with the bottom line,” says Garcia. “The way you need to address this as a hospital is to be more efficient with the care you’re delivering.” That means keeping patients out of the ER whenever possible and connecting with the community. “Address head on, at a very early stage, some of the problems that are so prevalent in these populations; [basic] things like diabetes, heart failure, and high blood pressure.”
Things are beginning to change at the state level, too. “[They’re] very adamant about moving us from a fee-for- service system to more of a managed care system,” says Garcia.
Garcia breaks down the economics of it. “If I’m going to be given a flat rate to take care of [the Medicaid population], I’m incentivized to do as much preventative care as possible because that reduces the cost of caring for those individuals and therefore gives me the highest chance of making a margin, which is important for me.” The key, Garcia says, is “rolling it all out in an intelligent way that doesn’t somehow reduce services for people. It is definitely the way healthcare’s going.”
Peace doesn’t see the issue as one of access to care at all. “Now, is it appropriate care?” she asks. Like so many other folks in the industry, Peace recognizes that many of her potential patients never reach her at all. Instead, they end up in the emergency room. And Garcia will tell you that, by far and away, that is the most inefficient and most expensive way to access to healthcare.
Published in Chicago Health Summer/Fall 2012