Chicago police officer undergoes first-ever double-lung transplant due to Covid-19 and cancer
The last time Arthur Gillespie spoke to his cousin was on his front porch in Beverly, but he didn’t realize they would never seen each other again. It was February 2020, and his cousin was experiencing Covid-19 symptoms.
Within weeks, his cousin had passed away, says Gillespie, a police captain with the University of Chicago Police Department. “It was frightening and at the beginning of the pandemic when we weren’t getting a lot of information. I knew people were going to the hospital and not coming home.”
Gillespie suffered two more losses due to Covid in the following months: his uncle and father.
He had his own battle with the virus, too. For about a week, Gillespie, 56, tried to manage symptoms at home, but he continued to deteriorate. He called an ambulance and stayed in the hospital for 12 days.
His time in the hospital didn’t end there, however. While undergoing tests, doctors detected a spot on Gillespie’s right lung.
From Covid hospitalization to cancer diagnosis

While the surgery went well, recovery was difficult. Gillespie hoped to get back in shape and back to work. But after three years of physical therapy and exercise, he began to lose hope.
“My symptoms were getting worse, and my oxygen levels were getting worse. When I would go to rehab and exercise, there came a point where I was plateauing and started to see regression,” he says.
Gillespie sought a second opinion at Northwestern Medicine in September 2023. The surgeon he met with informed him that he had pulmonary hypertension — a type of high blood pressure that affects arteries in the lungs and heart. His difficulties also stemmed from Covid damage to his left lung and cancer damage to his right.
In fact, the damage was so severe, Gillespie recalls the doctor saying that he only had one to two years left to live. He appeared physically strong, but he could barely speak a sentence without losing breath; he had to sit down after only a few steps.
Physicians also noted that the pressure within Gillespie’s lungs was so intense, it was causing heart failure. His only option: a double-lung transplant.
A rare situation
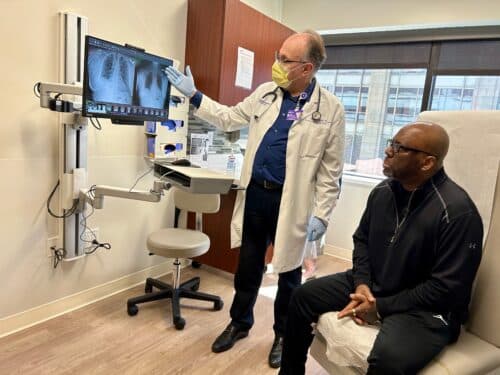
“Fortunately, we don’t see many more patients who are dying or on a ventilator from Covid, which is a good news. However, there are some patients who survive Covid but who have interstitial lung disease, which includes scarring on the lungs,” Tomic says. “This is what Arthur had.”
And he wasn’t the first. In June 2020, Northwestern’s thoracic surgery team performed the first-ever double-lung transplant on a woman in her 20s whose lungs Covid had irreversibly damaged.
Gillespie underwent a double-lung transplant in January of this year, through an observational study at Northwestern in which clinicians perform double-lung transplants and then continually monitor and evaluate their effectiveness.
Quick results
Gillespie says he noticed a difference in his breathing ability immediately after surgery. And once his surgery wounds healed, he was able to breathe on his own.
However, recovery continues to be a slow process: “Before this, I was an exercise and fitness buff. I’m trying to be patient and allow my body to recover and take it slow while regaining strength,” Gillespie says.
He also had to come to terms with accepting disability from his job, after working in law enforcement for 30 years.
“It was a hard thing to accept,” Gillespie says. “I thought once you hit that reality, it stays with you, but now my expectation is that I can improve my health to the point where disability will no longer be my status. That’s something I look forward to.”
Gillespie is happy to be a pioneer in providing this opportunity to others. He shares his story in hopes that others will pursue second opinions.
“Even when I didn’t think that recovery was going to be something that was realistic to me, I’m on the other side of that now. I’m actually living and recovering,” Gillespie says.
Above photos courtesy of Northwestern Medicine Media Relations.










