DXA Scanner. Photo courtesy of Northwestern Medicine’s Bone Health and Osteoporosis Center
For women facing a cancer diagnosis, there are countless questions that come to mind. From treatments and medications to the emotional journey of living with cancer, it’s easy for the mind to get full — and fast. The last question a woman is likely to ask, however, is an important one: What about my bones?
We sat down with June M. McKoy, MD, program director for the Geriatric Medicine Fellowship and attending physician with Northwestern Medicine’s Bone Health and Osteoporosis Program, to explore the correlation between bone health and a cancer diagnosis. We also dug into how Northwestern’s Bone Health program is working hand-in-hand with oncologists to help women proactively manage both a cancer diagnosis and their bone health.
What is bone health?
Bone health simply refers to the density of a person’s bones. If you think of bones as being made up of a lattice-type structure of minerals (which is exactly what they are), a healthy bone has a tightly-woven lattice structure — a high density. In someone with compromised bone health, however, that lattice structure has eroded and become more loosely woven and less dense. When bone health is compromised, the risk for fractures — even from mild injuries — increases. Osteoporosis kills more women than does breast cancer, McKoy says.
The link between cancer and bone health
Given that one in two women over 50 will face an osteoporosis-related fracture in her lifetime, bone health is of the utmost concern for women. And it’s particularly important for women dealing with cancer treatment. “The best treatments for a woman’s cancer can often be less optimal for her bones,” McKoy says. “It’s about striking a balance between the most effective course of cancer treatment while keeping bones healthy.”
Many common cancer treatments may put bone health at risk. Both radiation and chemotherapy treatments can compromise bone structure while attacking cancer cells. Hormonal therapies, especially for breast cancer, tend to have the greatest adverse impact on a woman’s bone health. This makes conversations about bone health between a woman facing cancer and her oncologist imperative, so that a life-saving treatment doesn’t put her bones at risk.
Often, bone health conversations aren’t made a part of a patient’s diagnosis and treatment options. Northwestern’s approach looks to change that. McKoy’s passion for bone health stems from a personal connection: a family member with a breast cancer diagnosis. While her relative received the life-saving oncology treatment she needed, she found her bone health compromised. This led McKoy to pursue the connection between cancer and bone health through the early stages of Northwestern’s Bone Health Program.
The program, housed in Northwestern’s endocrinology department, serves as a nexus for guiding women’s bone health from the beginning of a cancer diagnosis. This includes primary screenings and diagnostics, as well as blood tests to check vitamin D levels. Vitamin D affects the body’s ability to absorb calcium and deficiencies and can indicate compromised bone health. Additional blood tests might identify other underlying causes of decreasing bone health, such as multiple myeloma or thyroid disease.
Navigating cancer and bone health hand-in-hand
“The best time for a woman to start a conversation about her bone health is at the point of treatment,” McKoy says. “When she has her first appointment with her medical oncologist, just put the question out there: ‘What about my bones?’”
McKoy advises that patients ask their physicians how recommended therapies (such as hormonal therapy) might impact their bones and how they can prevent adverse effects from happening. Patients should also inquire how their physicians manage any adverse effects therapies might have on bone health and what the process will be for making bones strong again.
McKoy adds that talking about bone health in conjunction with cancer treatment puts women in the driver’s seat. “When you put that question out there, your medical oncologist has to answer it. It’s to everyone’s advantage.”
So how does Northwestern’s Bone Health and Osteoporosis Program work with women living with cancer? Along with two other physicians (Eve Bloomgarden, MD, and program director, Allison Hahr, MD), McKoy is certified by the International Society of Clinical Densitometry to read bone scans and interpret the results. The scans, which test bone density, are performed by a certified technician using an enhanced form of x-ray technology called a dual-energy x-ray absorptiometry (DXA) scanner to measure bone loss primarily in the spine and the hips.
Patients come into the Bone Health and Osteoporosis Program by physician referral, often from oncologists. On their first visit, women will complete an extensive personal health profile, which helps McKoy and her colleagues understand their family, medical and lifestyle history. This way, they can identify risk factors for bone health and determine whether a DXA scan is appropriate. Risk factors can include, but aren’t limited to, a family history of osteoporosis, lupus, ethnicity (highest in Caucasians and Asians) and a history of taking epilepsy medications (like Dilantin) and steroid medications (like Prednisone).
“The best time for a woman to start a conversation about her bone health is at the point of treatment”
Unlike other confining scans like an MRI or CT scan, DXA scans are performed in a small exam room with the patient fully clothed. At Northwestern, the DXA technician plays soft music in the background to put the patient at ease. The entire scan takes about 15 minutes, with no injections and no chalky contrast fluid to choke down.
What’s next for patients?
DXA scans can show a range of possibilities, from osteopenia (lower than normal bone density, but not yet osteoporosis) to osteoporosis. Both osteoporosis and osteopenia can be slowed and bone density improved. Recommendations will be made for courses of treatment that will help a woman restore her bone health. These can include dietary recommendations (like calcium-rich foods) and supplements.
But what about women not currently facing cancer who are concerned about bone health? Being proactive can start at any age. McKoy recommends that pre-menopausal women take 1,000 mg of calcium daily, along with 400 to 800 IU of vitamin D. For post-menopausal women, those guidelines adjust to 1,200 mg of calcium per day and 800 to 1,000 IU of vitamin D. Additionally, weight-bearing exercise is crucial to help improve bone density.
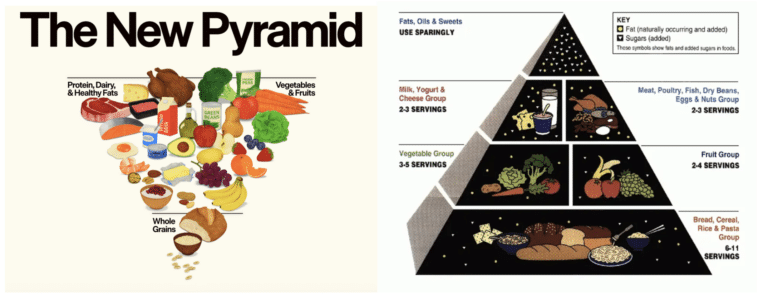
The best source for these additional vitamins and minerals? Food, of course — especially given that the body can only process a maximum of 500 mg of calcium at a time. Leafy green vegetables and dairy products are fantastic sources of calcium and vitamin D, respectively. Vitamin D is also added to some brands of orange juice, soymilk and cereal. And for those who can’t quite make up the entire recommended intake through food, the rest, McKoy says, can be taken through supplements.
For more severe cases of bone loss and advanced osteoporosis, Fosamax, Boniva, Actonel, Reclast, Evista, Prolia and Forteo are the most widely used medications that may be prescribed.
As with any health challenge, it takes incredible strength to face a cancer diagnosis. Better questions spark better conversations about treatment, and questions about bone health can empower women facing cancer to be stronger than cancer in every way possible.