Radioactive scans can save lives, but at what risk?
Over the past decade, the number of computerized axial tomography scans, better known as CT or CAT scans, has increased dramatically. But their widespread use also has led to questions about their safety.
“CT use has exploded,” says Dr. Daniel Appelbaum, director of nuclear medicine and PET/CT and associate professor of radiology at the University of Chicago Medical Center. “A lot more people are getting radiation exposure through CT scans. And some people are getting many, many scans.”
Between 1980 and 2006, the annual radiation dose from medical procedures increased sevenfold. With the increased use of CT scans, has come well-publicized examples of their misuse, such as when some hospitals, including Cedars-Sinai Medical Center in Los Angeles, used dangerously high levels of radiation during CT brain perfusion scans, causing a ring-like hair loss. Other centers have exposed patients to extra radiation by giving them double chest CTs; one with iodine contrast and one without, when one scan is all that is necessary.
“All of these [high-profile events] the last couple of years have been a bit of a wake-up call to radiologists and imaging physicists that we have to get a better handle on this,” Appelbaum says.
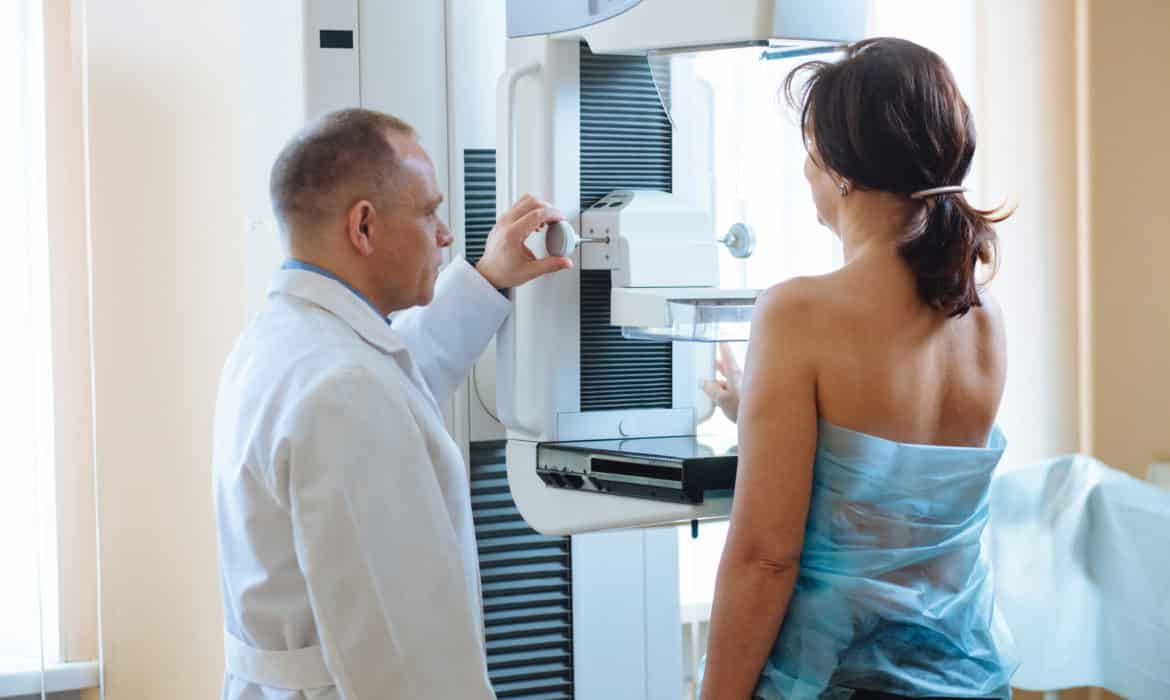
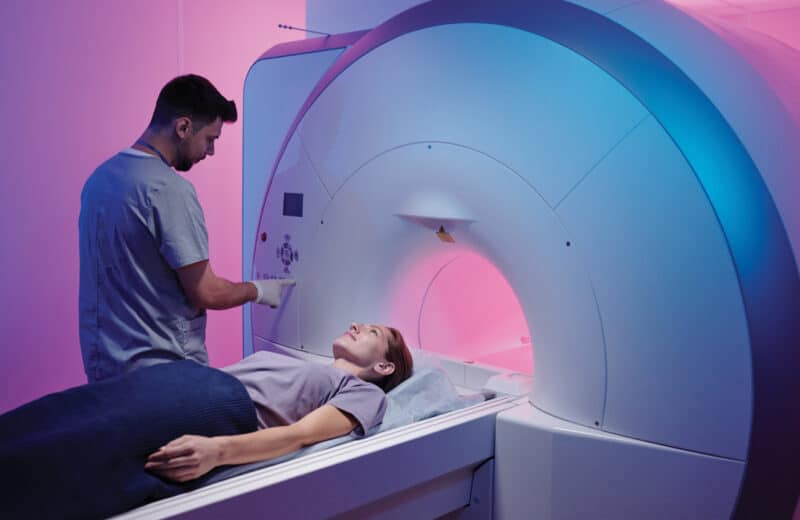
CT scans using ionizing radiation, a category of radiation that also includes X-rays, mammograms, and positron emission tomography (PET) scans, can increase a patient’s risk of developing cancer. By contrast, nonionizing radiation—such as the sound waves used in ultrasound and magnetic resonance imaging (MRI), which uses radio frequencies and magnetic fields—pose almost no risks.
The American Cancer Society reports, “Most scientists and regulatory agencies agree that even small doses of ionizing radiation increase cancer risk, although by a very small amount.”
Properly indicated, properly performed scans are safe, Appelbaum says. “If the exam is medically indicated, the medical benefits of having the exam far outweigh the radiation risk. It can be far riskier not to get the scan. [With a properly indicated CT scan] you’ll see that a patient has an aneurism about to rupture, or a smoker comes in with a cough, and you’ll see the lung cancer when it’s still curable.”
The risk of a single CT scan causing cancer 10 or 20 years later is about 1 in 1,000 for women and 1 in 2,000 for men, though it depends on the type of CT scan. It’s a negligible risk, medical professionals say, considering that the general risk of any individual getting cancer in his or her lifetime is 1 in 5.
Still, the profession is buckling down and instituting tighter standards. “As a radiology community, we have not always been sensitive to this issue or proactive to really minimize the amount of patient radiation exposure,” Appelbaum says. Now that’s changing, he says, with the American College of Radiology’s Image Wisely (for adults) and Image Gently (for kids) campaigns that encourage radiologists to develop protocols that use the lowest acceptable radiation doses. Radiologists are more careful with children, since radiation is even more harmful for kids.
“The more X-rays you use, up to a point, the prettier the pictures,”
Appelbaum explains. “In the past, it was ‘How pretty can you make the picture?’ Now it’s ‘How ugly we can get away with? What’s the least amount of radiation we can use?’ We also really want to push the envelope for ‘How low can you go?’ with kids to minimize their radiation exposure.”
With the advent of electronic medical records, a medical center can track how much radiation exposure individual patients have had, though there’s currently no easy way to track it across medical centers.
NorthShore University HealthSystem monitors the radiation exposure of patients to determine whether a patient is getting too much cumulative radiation exposure. If the threshold is too high, radiologists may talk to the referring physician to suggest an alternate test like an ultrasound or MRI.
“We don’t want a situation in which a patient gets 20 CT scans, and we don’t know about it. That’s unacceptable,” says Dr. Robert Edelman, chairman of radiology at NorthShore and professor of clinical radiology at Northwestern University Feinberg School of Medicine. “We want this to be an important part of the medical record, so we don’t unintentionally cause harm to the patient.”
It’s a question of relative risk, says John Hibbeln, MD, director of CT imaging, vice chairman of diagnostic radiology and radiation safety officer at Rush University Medical Center. “My goodness, crossing the street is a risk. How do we minimize the risk of crossing the street? We cross at the corner; we look both ways. The same is true for [minimizing] the risk from diagnostic imaging,” he says. “A lot of the hysteria is causing problems. We have people refusing diagnostic studies and putting themselves at risk. There’s very little talk about the benefits.”
If a patient has a CT scan for a gunshot wound or a stroke, Hibbeln says, the 1-in-1,000 chance of causing cancer in 20 years is a low risk. “But the benefit of finding cancer, finding blood vessels that are blocked or intestinal perforation—that’s a real benefit. Do we not do the study because they might get cancer in 20 years? To have that risk of dying right now?” he asks.
Edelman emphasizes that, despite potential concerns about radiation exposure, CT is a valuable test when used appropriately. “It benefits patients by enabling a faster and more accurate diagnosis and is often life-saving for patients suffering from trauma and other medical emergencies,” he says. “Generally CT helps the physician obtain the best health outcome for the patient.”
Published in Chicago Health Winter 2012