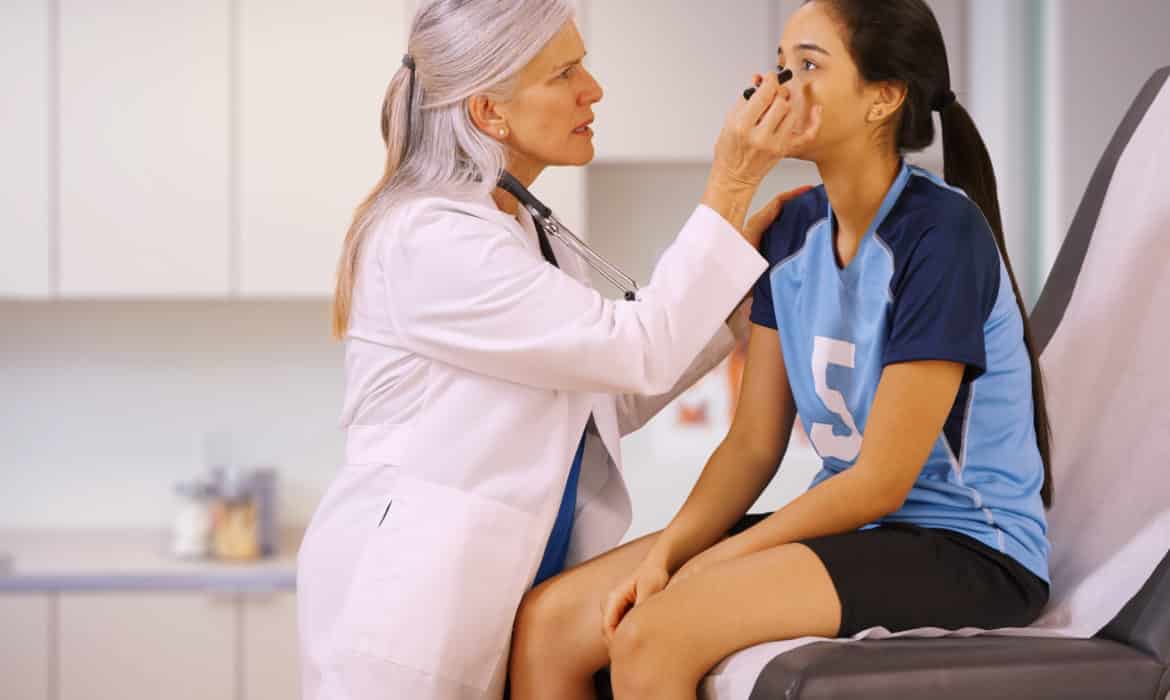
During a scrimmage for high school soccer tryouts, right freshman defenseman Andrew Devendorf and a teammate jumped to head a ball in the air. It’s a standard action in the sport to redirect or gain possession of the ball, but it’s also among the most dangerous. Instead of making contact with the ball, Devendorf and his teammate collided skulls.
“I remember landing cleanly on two feet, then wobbling like a top and falling to the ground,” Devendorf says. “I had the worst pain in my head. A throbbing, like my head had a thick pulse.”
The scrimmage was stopped, and Devendorf was helped off the field. He was taken to the hospital, where he was given a CT scan and diagnosed with a grade three concussion — the most severe type.
“The whole time I didn’t think anything was wrong with me. I had this terrible pain, but it never occurred to me that I had a concussion,” Devendorf says.
A concussion is a traumatic brain injury (TBI) caused by a blow or jolt to the head or a hit to the body that causes the skull and brain to jostle as if shaking a Magic 8-Ball toy. In 2013, there were about 2.8 million TBI-related hospital visits in the U.S., according to the Centers for Disease Control and Prevention (CDC). Awareness of concussions has been growing, and now treatments are changing too.
Symptoms of a concussion range from a throbbing headache to brain hemorrhaging, which can begin immediately or days after impact.
Physical therapist Julie O’Connell, PT, ATC, director of performing arts rehabilitation for Athletico Physical Therapy, cites blurred vision, headaches and nausea as common concussion symptoms. “In some athletes, their equilibrium is off,” she adds.
For years, youth athletes diagnosed with a concussion were given a brain CT scan and told to follow a desensitization protocol, which O’Connell describes as an environment with no electronics and low amounts of stimulation. “They were taken out of school for an extended period and asked not to do a lot of reading or anything stimulating,” she says. “Basically, to give the brain a rest.”
But this approach is now changing. This fall, the CDC introduced sweeping changes to protocols for pediatric concussion diagnosis and treatment. Gone is the go-to use of expensive and unnecessary brain CT scans to check for concussions. Also, after two to three days of rest, patients can gradually increase their activity and return to non-sports activity.
Skipping routine pediatric CT scans, which deliver radiation, is something Marc Hilgers, MD, a sports medicine physician at Advocate Medical Group, has long been advocating for.
“This is a really big step that the CDC took,” Hilgers says. “Forgoing the routine image scanning unless there are red flags is significant because we’ve seen the effects of radiation on a kid with a brain that is still developing.”
Hilgers cites a study in the The BMJ charting the long-term effects of radiation on kids’ brains as they mature into adulthood. Children who had been given low doses of radiation in infancy scored lower on tests of learning ability and logical reasoning as young adults.
“Radiation of a maturing brain is dangerous,” Hilgers says. “Therefore, unnecessary exposure — for whatever reason, including imaging for concussions — should be avoided if possible.”
The treatment protocol is also changing to get patients back to light activity.
“They basically diagnosed me and told me to rest and stay off the field for two weeks,” Devendorf says. “The pain was there for the first two to three days,” he says, but it got better quickly after that. “It was frustrating to just sit around because I felt physically fine.”
Devendorf was instructed to completely rest for two weeks — something Hilgers and the CDC no longer advise. It’s now recommended that kids gradually return to physical and mental activity after two or three days of rest. “We want kids to read a book or take a light a jog,” Hilgers says. “Something that gently increases heart rate and elevates blood pressure will help the athlete come back faster and more efficiently.”
Many young athletes don’t seek treatment because they don’t want to be removed from competitive play. “There’s lot of hiding of symptoms,” O’Connell says. “Athletes don’t often want to come forward and admit they are feeling concussed.”
The drive to compete despite such a serious head injury stayed with Devendorf, even after he suffered two more concussions: a second as a sophomore and a third as a junior.
“The thing most on my mind was never that I had a concussion, but that I couldn’t play games. The first time I had one, I had made the soccer team, but I was competing for a starting spot on the team. The second time, I had to miss an entire week of games.”
Preventing concussions from happening in the first place remains a high priority, with changing rules in youth sports. But concussions are hard to prevent, and they can occur anywhere and to anyone, making proper diagnosis and treatment important.
Ultimately, the onus is on everyone to help athletes be head smart. “Adults, referees, the rules, legislation and committees — we all need to keep athletes safe,” O’Connell says.
RESOURCES: