Advances help age-related macular degeneration
Just because you can read the words on this page now doesn’t mean that will always be the case. An aging population in the United States is facing an ocular health epidemic—but many people don’t yet see the problem.
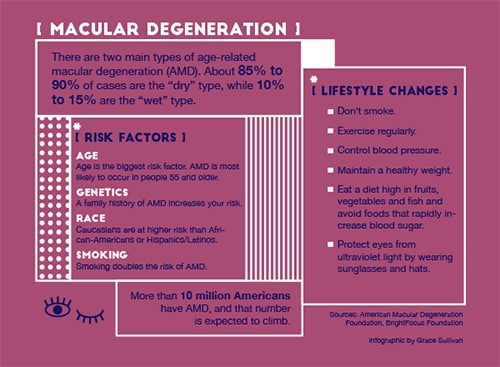
Age-related macular degeneration (AMD) causes vision loss in more people than cataracts and glaucoma combined. More than 10 million Americans have AMD, and that number is expected to climb, according to the American Macular Degeneration Foundation.
With AMD, the retina deteriorates over time, causing people to lose the ability to see the center of their vision. “With advanced dry AMD, parts of your vision start to disappear, like erasing part of a chalkboard so that the writing is missing. You may develop a black spot in the center where you see nothing. With advanced wet AMD, you may get distorted, blurred or missing areas in the center of your vision,” says Jennifer Lim, MD, professor of ophthalmology and director of Retina Service at the Eye and Ear Infirmary at the University of Illinois at Chicago.
Sharon Marshall knows the feeling. The 71-year-old DeKalb resident was diagnosed with the dry form of AMD in her mid-60s and the wet form a few years later. AMD runs in Marshall’s family, and she watched two of her aunts suffer with it. “They were diagnosed too late. They didn’t have much vision left as far as seeing faces and reading.”
Often patients become devastated upon diagnosis because they think of the experiences of past generations, says Vikram Setlur, MD, a retina specialist at the Wheaton Eye Clinic. However, treatment continues to improve. “I’m confident that with new drugs in the pharmaceutical pipeline, treatment will get better and better,” he says.
Disappearing Sight
Not every case of AMD is the same. The dry form of the condition accounts for the vast majority of cases—85 to 90 percent—while the wet form makes up the rest. And in some cases, like Marshall’s, dry can progress to wet.
Dry AMD happens when the retina thins out and becomes less functional. In the wet form, blood vessels grow behind the retina, become leaky and cause fluid to collect and blisters to develop.
Vision exams can help spot problems. “That’s why everyone 55 and older needs an annual eye exam,” Lim says.
An ophthalmologist looks for signs of AMD, such as scarring and changes in pigmentation—tiny yellow or brown spots. Patients with wet AMD will show blood, blisters or fluid in the retina.
The ophthalmologist may refer the patient to a retina specialist, who conducts further tests. One of those tests—optical coherence tomography—uses light waves to create high-resolution images of the retina. Based on these images, patients are given a risk score of one to four, taking into account the disease’s progression.
Individuals often don’t notice changes in their sight until the intermediate or late stages of the disease. Unfortunately, the further the disease progresses, the harder it is to treat.
“Even if you’re seeing well and don’t wear glasses, it’s important to have an eye doctor make sure your eyes are healthy from front to back,” Setlur says.
Who’s at Risk?
A person’s risk depends, in part, on lifestyle and genetic factors. Caucasians are more likely than other races to develop AMD—about 30 percent will develop the disease by the time they are in their 70s, Lim says. Researchers have identified some 20 genes that put people at greater risk for macular degeneration, according to the National Eye Institute. Individuals with a family history also run a higher risk.
Lifestyle factors include smoking (which doubles the risk of AMD), high blood pressure, high cholesterol, unhealthy diet and lack of exercise. UV light exposure and environmental factors may also play a role.
Lim says that she is up front with her patients who smoke, explaining that their choice could lead to a higher risk of advanced forms of AMD as well as blindness. “That gets them. They don’t want to go blind,” she says.
The Bright Side
While it’s not possible to reverse vision loss from AMD, there are ways to slow its progression.
The only treatment for the dry form of AMD is nutritional therapy. The National Eye Institute reports that high levels of antioxidants and zinc reduce the progression of AMD. In 2013, researchers in the Age-Related Eye Disease Study 2 (AREDS-2) refined their suggested supplements to include:
• 500 mg vitamin C
• 400 IU vitamin E
• 80 mg zinc
• 10 mg lutein
• 2 mg copper
• 2 mg zeaxanthin
Look for supplements labeled with the AREDS-2 stamp of approval, adds Jon Gieser, MD, a retina specialist at the Wheaton Eye Clinic. Also, control lifestyle factors. “Some of the most effective preventative measures are simple ones that all of us know we should be doing anyway—eating a healthy diet, watching cholesterol and blood pressure, and exercising,” he says.
For people with wet AMD, treatments include injections to inhibit the formation of blood vessels in the retina and laser surgery to seal leaking blood vessels.
“The key is to get it early. If the patient is diagnosed with wet AMD, they’re usually getting their first treatment that day or in the next few days,” Setlur says.
For Gieser, who runs AMD clinical trials, hope might lie in detecting a person’s susceptibility to macular degeneration before the disease develops. “We’ll have preventative measures that can forestall onset, and I hold out hope that we will have therapy for patients with dry macular degeneration,” he says.
Lim is hopeful, too. “It’s really amazing what we can do for patients in 2016. Maybe in my daughter’s generation [we’ll] reverse the problem. It’s going to be a different world out there.”