How the da Vinci robot is changing the face of surgery.
The idea of machines conducting procedures on human beings has been a stronghold in science fiction for a while. We’ve seen the imagery countless times in books, on television and in movies. But only in the last decade has this futuristic vision become a day-to-day reality.
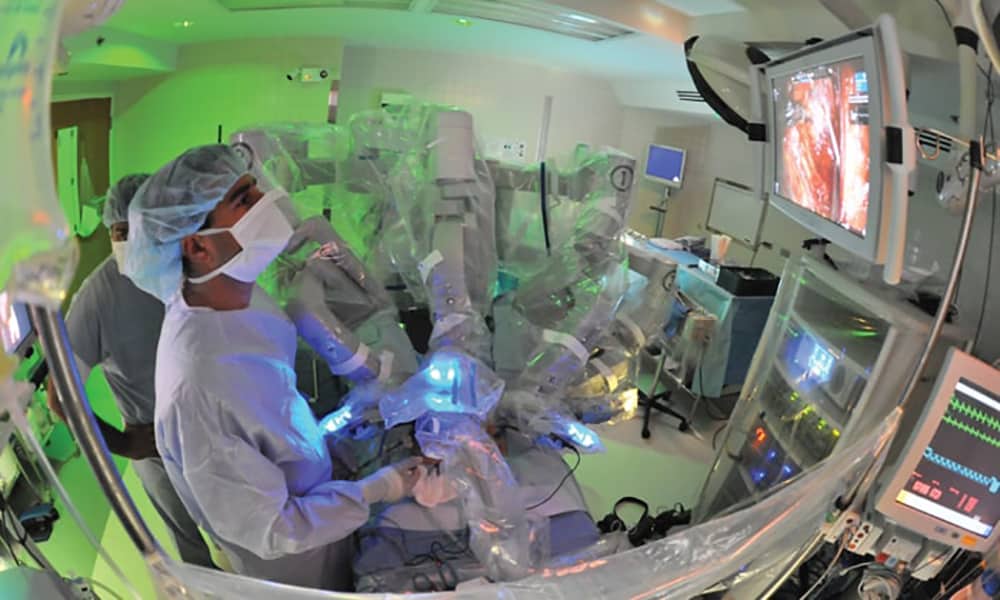
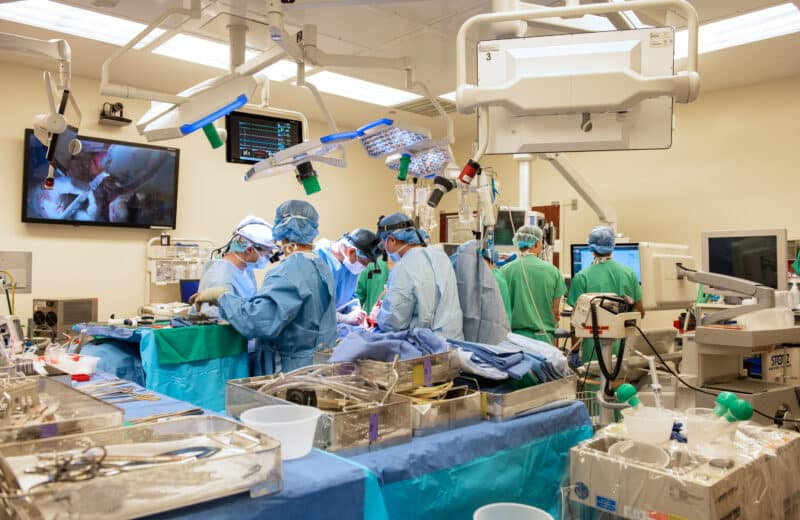
In hundreds of hospitals around the world, the da Vinci Surgical System looms over patients’ beds resembling a giant mechanical spider-like bug (although it only has up to four arms). During surgery, the patient all but disappears beneath the machine; its long articulated instruments inside the patient’s body snipping and suturing away; miming in miniature the movements of a surgeon seated at a console across the room. From here, the surgeon is provided a magnified, 3-D image of the patient by the da Vinci’s laparoscopic camera.
It was only a few years ago that Dr. Mohan Gundeti, director and chief of pediatric urology at Comer Children’s Hospital at University of Chicago, became the first surgeon in the world to perform a pediatric bladder reconstruction surgery using the da Vinci robot. His patient, Aaliyah Dellar, then 10 years old, had a bladder that was too small and would often have uncontrollable spasms. If Gundeti used conventional methods, Dellar would have been left with a six-inch scar running from above the bellybutton down into the pubic area.
Whenever you make a big incision, you are cutting the muscles. And when you cut the muscles, more time is needed to heal,” says Gundeti.
Gundeti proposed using the da Vinci robot. Dellar’s mother Paula Thigpen says that at first she was surprised, but she was soon on board with the idea. “I was actually kind of relieved because it was less invasive. [It] gave Aaliyah a great opportunity for a speedy recovery and a better quality of life.”
Gundeti explains that a major benefit of the robot is the prevention of fluid loss. “Because you’re doing everything inside the abdomen, and you’re not opening anything; there is less indirect loss of water, and blood loss is minimal because you’re doing everything in a specialized environment.”
The successful surgery provides Dellar with greater bladder control. That would be important to anyone, but for a young girl, it’s essential. “Kids can be mean,” says Thigpen. “It kind of puts you in a shell because you always have to be mindful; you could have an accident at any moment.”
Today, Dellar is a dancer, something she never would have been able to do before the surgery. “Flips and jumping and splits—that stuff was all out of the question,” says her mother. “It really changed her life quite a bit.”
The da Vinci robot was developed by Intuitive Surgical Inc. and introduced in 1999. Manual laparoscopic devices had been in use for some time, but the robot was an innovation unlike anything anyone had seen before.
Dr. Frank Tu, division director for gynecological pain and minimally invasive surgery at NorthShore University HealthSystem describes the experience of working with the robot as similar to “playing a video game.”
“There’s a long history of doing minimally invasive procedures in women’s health; it dates back 30 some years,” Tu says. “The robotic-assisted approach has captured the imagination of surgeons, much more so than the already existing strategy of a straight laparoscopic approach.”
At the NorthShore Kellogg Cancer Center, surgeons have found that the da Vinci system can be a real asset in uterine cancer staging (the process in which doctors determine how far a cancer has spread). Many surgeons believe that the da Vinci “provides the best physical assistance,” says Tu.
“The preference for the robot has a lot to do with the philosophy and training of the individual surgeon,” Tu explains. Hysterectomy, or even simpler procedures such as tubal sterilization or ovarian cyst removal, can be easily performed by experienced surgeons like Tu and his partners using less expensive endoscopic instruments. But the allure of the robot is strong. Though it isn’t currently a necessity for gynecology, count on seeing more of these machines popping up in hospitals and doctors offices across the country.
Robotic-assisted surgery may not be revolutionary to the approach of gynecological procedures, but when facing prostate cancer, a disease that affects one in six men, the robot has changed the face of the game.
“About 70 percent of prostate cancer surgeries are done robotically, and that will continue to grow,” says Dr. Kalyan Latchamsetty, a urologic surgeon at Rush University Medical Center.
“With the traditional technique of laparoscopic surgery, it is much more difficult to remove the prostate gland for prostate cancer because of its location deep within the pelvis,” says Latchamsetty. “The robotic instruments make the surgery much easier to perform.
“Specifically, it is much easier to suture deep in the pelvis with robotic instruments compared to traditional laparoscopic instruments. Especially when we perform anastomosis, [connecting] the bladder to the urethra,” he says.
The feel of surgery is lost to a great degree when using the da Vinci robot. And some surgeons value the sense of touch associated with open surgery.
“You do lack tactile sensation with the robotic system; that’s something that the developers are working on now,” Latchamsetty says. “But the visualization more than makes up for the lack of tactile sensation. We have an excellent 3-D image of the pelvis with robotic surgery. We can see much better than with open surgery—especially deep in the pelvis.”
“At Rush, we offer both the open and robotic surgery for prostate cancer,” says Latchamsetty. “I strictly offer the robotic approach because of my experience with it and excellent patient outcome.”
There is also the issue of cost. The system is not cheap, and the robot has a lot of expensive, single-use parts that must be replaced after every procedure. But avoiding a scar and gaining a faster recovery are worth a great deal to many patients.
Gundeti sees it this way: “The family can spend less time in the hospital and less time helping [the patient] to recover at home. So we are saving some dollars and helping the family to get back to work.”
For Gundeti’s former patient, Aaliyah Dellar, her mom says she’s busy “being a regular teenager. She’s a freshman in high school now. She went to her first homecoming dance. She loved it; she said she danced all night.”
There are some things you can’t put a price tag on.
Published in Chicago Health Winter 2012